Seeing as cosmetics can be a complex mixture of substances, it is inevitable that some of them produce allergies to certain people. Symptoms of cosmetics allergy can occur after using a new cosmetic product, or even if you’ve been using one for years without an issue. One type of reaction is damage to your skin which can then burn, itch, sting, and get red. The second type of reaction is triggered by your immune system and can cause swelling, redness, and itchiness.
Both of them sound quite similar and are hard to distinguish, they can even be a combination of the two! In order to avoid cosmetics allergy, you can try testing a product by applying it to a small area of your body and leave it for up to 72 hours to check if you’ll get a reaction. If you use fragrances, apply them to your clothes, not your skin. You can even look for products with as fewest ingredients as possible, thus reducing the risk.
Would you like to know more? Read below the article by Dr. Philipp Spring.
COSMETICS ALLERGY: INTRODUCTION
Along with fragrance mixtures, preservatives are the allergens most frequently responsible for allergic contact eczema after external application of a product. Preservatives are not only used in industry (coolants, cleaning agents), they are also present in cosmetics in particular. Because of their allergenic properties, which have been discovered in recent years, certain substances have already come under closer scrutiny by the health authorities.
WHAT IS MEANT BY PRESERVATIVES?
It is a molecule added to a product, either industrial or cosmetic, to prevent its natural (physical or chemical) decay. Some preservatives are antimicrobial (antibacterial, antifungal), while others are true antioxidants. They are also found in medicines and foods. Some are also found naturally in fruit or plants.
WHAT HAPPENS IF YOU ARE ALLERGIC TO PRESERVATIVES?
The application of these chemical substances to the skin leads to “sensitisation”. The immune system skin perceives the molecule as an external aggressor and gradually conditions itself against it. In this case, the substance is called an “allergen”. As in the case of a nickel allergy, the preservatives cause an immunological reaction in the cells, i.e. a delayed (retarded) reaction with a clonal multiplication of the T-lymph cells in the lymph nodes. As a result, an ever smaller concentration of allergen causes an ever more violent inflammation of the skin: this is the so-called allergic contact eczema. It is not fatal like anaphylactic shock, which is an immediate reaction, but it is still very debilitating.
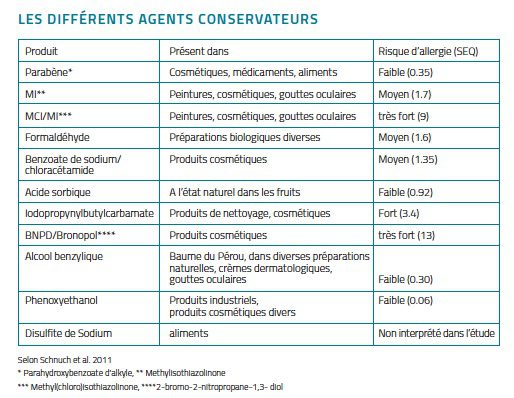
It usually affects the hands, regions of the face and décolleté (industrial products, creams) or the ears and scalp (hair sprays, hair lacquers, shampoo). An allergy is therefore the risk of developing a “sensitisation” to a product that is related to the frequency of use of the product. The more ubiquitous the substance, the more exposed the consumer. For this reason, the scientific literature has established a quotient (SEQ= Sensitization Exposure Quotient). The higher the quotient, the higher the risk. Preservatives present in food and medicines do not pose the same allergological problem, because it is the external application that triggers eczema.
WHAT DIAGNOSTIC TESTS ARE NEEDED?
To help the patient identify the product causing the eczema, an epicutaneous test is indicated. The suspected substances are applied to the patient’s back and fixed for 48 hours. This is followed by the first reading. After another 48 hours, a second reading is taken by the specialist to determine the allergic reaction. If erythematous, vesicular or sometimes weeping lesions appear after 96 hours, the result is interpreted as positive. At the same time, the standard series of classic allergens nickel, cobalt or bichromate is tested to rule out fragrance allergy. The test series of preservatives is regularly updated.
WHAT IS THE THERAPY?
Once the allergen is identified, the patient must be diligent in ruling it out. He must check the packaging to see if the identified trigger is present in the product. He can do this with the help of the allergy passport and the information sheet he received from the specialist. If the causative agent is consistently excluded, the eczema will disappear after a few weeks. Local application of group I/II corticosteroids to the face and genital area and group III/IV to the rest of the body allows for faster healing.
CONTACT ALLERGY EPIDEMIC AGAINST METHYLISOTHIAZOLINONE
Since the early 2000s, the preservative biocide methylisothiazolinone (MI) has been used as a substitute for the largely demonised parabens. However, the latter have a very low allergenic potential. Cases of isothiazolinone contact allergies, both cosmetic and occupational, have risen dramatically in all European countries. It is a real epidemic, but one over which the bodies responsible for cosmetovigilance are increasingly gaining control. Since 2017, there has been a European law imposing a cosmetovigilance concentration of 15 ppm (low) for rinse-off products and a total ban on products that remain on the skin.
SKIN FEELINGS
As soon as the cold season arrives, your child may feel an uncomfortable tightness on the lips, arms, stomach, flanks or thighs. You will then discover red patches surrounded by areas of dry skin. This eczema is most common in atopic children (dry skin, food allergies, hay fever). The associated itching causes eczema by scratching with possible bacterial and herpes infections. This vicious circle makes nights uncomfortable for the whole family.
HERE ARE 10 PRACTICAL TIPS TO OPTIMISE SKIN COMFORT:
- Take short baths with lukewarm water
- Avoid soaps, strongly scented and foaming shampoos
- Use only gentle washing creams and bath oils
- After longer stays in water such as. After longer stays in the water, e.g. in swimming pools/thermal baths (chlorinated water) or after a long bath, apply a body lotion, cream or balm depending on the degree of dryness
- Reduce the use of washing powder to a minimum and avoid fabric softeners
- Avoid synthetic clothing, wool, prefer cotton
- For babies and toddlers, it is advisable to remove the baby bodysuit, Wear pyjamas at night (avoid loss of trans-epidermal water)
- Keep the bedroom cool
- Ensure a balanced climate in the family so as not to put additional stress on children If, despite these measures, the situation does not improve or even worsens, do not hesitate to consult a dermatologist.
Author:
Dr. Philipp Spring
Epalinges medical center and dermatology department of the CHUV, Lausanne




